What Happens to the Brain with Concussion / TBI?

The brain is normally protected by the bony skull and insulated from jarring by
fluid that cushions the brain during movement. When the head or body
experiences any sudden movement (i.e. whiplash) the brain movement can
overcome the fluid cushion and be stretched, damaging nerves and become
bruised by bumping into the inside of the skull. These tissue injuries
disturb the transmission of nerve signals causing pain, dysfunction and
symptoms.
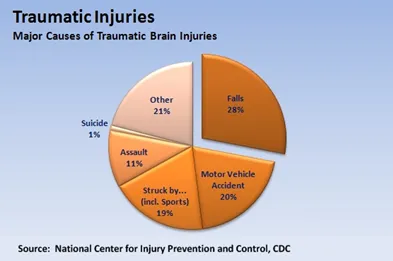
Some common ways to get a concussion / TBI are from
car accidents that result in whiplash, sports injuries and falls. Most
people sustaining a mild concussion, with appropriate care will
generally recover fully within weeks or months. Recovery may be slower
for older adults, young children and teens. More serious concussions or
repeated concussions often take longer to recover and may lead to
long-lasting problems with thinking, communicating, learning and
movement.
Some
symptoms may appear right away, while other symptoms may not appear for
days, weeks or even months after the injury. Some symptoms may not show
up until the person begins to resume their everyday activities, and when
additional demands are placed upon themselves. Sometimes people may be
unwilling to admit that they are having a problem or may not recognize a
problem. They can become angry, frustrated and/or confused about what
is happening to them. They may think they are okay even though they are
behaving differently. It is important that family members and others
acquainted with the person assist in pointing out changes in symptoms
and behavior to the doctor.
Young Children and Concussion
- Young children may have the same symptoms as adults, however may be harder to diagnose because of their inability to communicate. Symptoms listed below may indicate a concussion/ TBI:
- Crying more than usual
- Changes in the way the act or play
- Changes in nursing, eating or sleeping
- Becoming easily upset, exhibiting more tantrums
- Loss of new skills, such as toilet training Lack of interest in favorite toys
- Loss of balance and trouble walking
Older Adults and Concussion
Concussion / TBI in older adults are often missed and can be dangerous
if not addressed quickly. Identifying a serious problem may include
sudden onset of headache, increasing confusion or other symptoms
previously not expressed.
How is Concussion / TBI Diagnosed?
Any person suspected of having a concussion / TBI needs to see a
doctor. The doctor will ask series of questions related to the injury to
determine how the person's brain is currently functioning. Some
questions will test your ability to pay attention, solve simple problems
and how your memory is working. Other tests will include balance and
movement through space. The doctor will also check your strength,
reflexes, and sensation.
Additional tests may be ordered
depending on responses during initial examination. Imaging testing such
as CT scan and/or MRI of the brain may also be done to ensure there is
no internal bleeding or other damage. Neuropsychological tests may also
be ordered to evaluate how well you are processing information, if you
have memory deficits, language difficulties or if there is impairment of
your organization and planning abilities.
How is Concussion / TBI Treated?
The best way to recover from a concussion / TBI is to see a functional
neurology doctor specializing in concussion / TBI and whiplash. The
functional neurology doctor will examine you to determine how your brain
and nervous system are working and where nerve disruption is occurring.
This will ensure early diagnosis, appropriate treatment, timely
referral and implementation of a concussion / TBI self-management plan.
Functional Neurology methods provide immediate “real time biological
feedback” from your brain and body sowemaydesign a customized program of
care for your specific needs. We will then refine your program of care
each visit to accelerate your healing, break free of symptoms and allow
you to get on with your life.
Concussion / TBI symptoms may
appear mild, but without appropriate diagnosis and treatment can lead to
significant, life-long impairment affecting an individual's ability to
function physically, cognitively, and psychologically.
Centers for Disease Control and Prevention (CDC)
Concussion / TBI Self-Management Planning includes:
Following all recommendations of your functional neurology doctor.
Getting plenty of sleep at night, and taking it easy during the day.
Use ice or a cold pack on any swelling for 15 at a time with 15-30
minutes in between the next application. Always put a thin cloth between
the ice and your skin.
Ask your doctor when it's okay for you to drive a car,
Avoid activities that are physically demanding such as housework,
exercise, riding a bike, operating machinery and strenuous labor.*
Avoid activities that are mentally demanding such as schoolwork, video games, text messaging, or using the computer.*
*Your doctor may require you to take time off from work if necessary or change your school or work schedule while you recover.
Avoid alcohol and illegal drugs.
Take only prescription medications and over the counter medications as
directed by your physician or functional neurology doctor.
- Ibuprofen or acetaminophen: These medicines decrease pain. They are available without a doctor's order. Ask your functional neurology doctor which medicine is right for you. Ask how much to take and how often to take it. Follow your functional neurology doctor’s directions.
- These medicines can cause stomach bleeding if not taken correctly. Ibuprofen can cause kidney damage. Donottake ibuprofen if you have kidney disease, an ulcer, or allergies to aspirin. Acetaminophen can cause liver damage. Do not drink alcohol if you take acetaminophen.
- Take your medicine as directed. Call your functional neurology doctor and or primary care doctorif you think your medicine is not helping or if you have side effects. Tell him/her if you are allergic to any medicine. Keep a list of the medicines, vitamins, and herbs you take. Include the amounts, and when and why you take them. Bring the list or the pill bottles to follow - upvisits. Carry your medicine list with you in case of an emergency.
|
RED FLAGS |
